Facial Feminization Surgery Procedures
FFS includes a wide range of reconstructive and aesthetic surgical procedures that work to reshape facial features to make them appear more feminine. Depending on your current features and expectations you may need one or several of the following procedures to obtain the results you’re seeking:
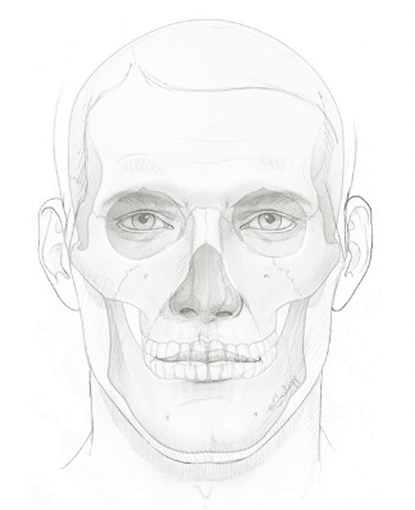
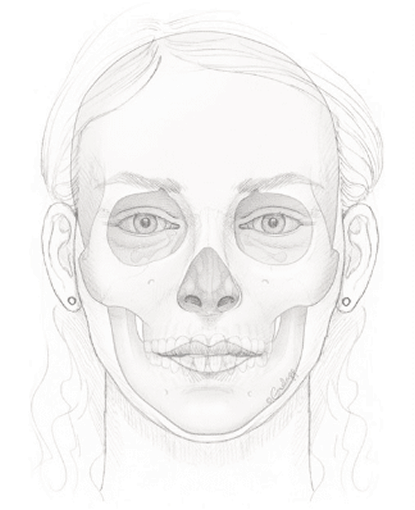
The Beginnings of Facial Feminization & Gender Confirmation Surgery
Prior to the advent of gender confirmation and FFS, individuals who suffered from gender dysphoria had no viable medical or surgical options. They could “dress to pass” as the gender they identified with but were still often seen by the world at large as their assigned gender-at-birth. Transgender women often lived with a deep sense of dissatisfaction and feeling uncomfortable in their own skin — physically, emotionally, and psychologically.
Another Shot At Facial Feminization Surgery
Have you had FFS surgery before but are less than happy with the results? Unfortunately, one of the most common types of facial gender confirmation procedures we perform is to correct a previous surgeon’s work. This is often because while a surgeon may know technically what is required for facial feminization, they may not understand the subtle qualities of what truly makes a face “feminine” versus what makes a face simply beautiful. To capture authentic feminine gender expression, your surgeon needs to fully comprehend the science and structural proportions behind male vs. female faces, and also have a deep awareness of the more subtle aesthetic qualities of what constitutes gender.

Facial Feminization Surgery: The Journey to Gender Affirmation
Dr. Deschamps-Braly’s book “Facial Feminization Surgery: The Journey to Gender Affirmation” is back and available now. This second edition covers advances in facial feminization, as well as helpful patient stories, and is a great resource for FFS patients and their loved ones.
Order Copy On Amazon
FAQs About Feminization Surgery
- Why Choose a Plastic Surgeon with Craniomaxillofacial Training for Your FFS?
- Can I Have a Facelift at the Same Time As My Facial Gender-Affirming Surgery?
- How Long Will the Surgery Take? How Safe Is Long-Format Surgery?
- Can I Do My FFS in Different Phases? Or Should It Happen All at Once?
- How Long Will It Take to Recover From Facial Gender-Affirming Surgery?
Download Our Facial Feminization Guide
Download Guide









